News and Announcements
Read the latest news from Northwestern University Feinberg School of Medicine’s Department of Preventive Medicine. The links below take you to articles where you can learn more about our faculty’s latest achievements, awards and honors.
 05.19.2026A team at the Robert J. Havey, MD Institute for Global Health, in collaboration with Mobile Imaging Innovations, Inc, a Chicago-based company, has developed an artificial intelligence (AI)-enabled smart microscope platform specifically designed for use in low-resource environments.
05.19.2026A team at the Robert J. Havey, MD Institute for Global Health, in collaboration with Mobile Imaging Innovations, Inc, a Chicago-based company, has developed an artificial intelligence (AI)-enabled smart microscope platform specifically designed for use in low-resource environments. 05.12.2026
05.12.2026A time-restricted eating program promoted greater weight loss in women with polycystic ovary syndrome (PCOS) than no intervention, according to a randomized controlled trial published in Nature Medicine.
 04.21.2026
04.21.2026Individuals exposed to adverse neighborhood social factors in early adulthood demonstrated a higher risk of developing coronary artery calcification in midlife, a key measure of early cardiovascular disease, according to a recent study published in Nature Communications.
 04.16.2026The Department of Preventive Medicine's Milkie Vu has been selected to join the newest class of William T. Grant Scholars. Launched in 1982, the William T. Grant Scholars Program has supported the professional development of over 200 talented early-career researchers.
04.16.2026The Department of Preventive Medicine's Milkie Vu has been selected to join the newest class of William T. Grant Scholars. Launched in 1982, the William T. Grant Scholars Program has supported the professional development of over 200 talented early-career researchers. 03.10.2026
03.10.2026Implementing an automated urinary incontinence screening and educational program in primary care practices significantly increased awareness and treatment referrals in women with the condition, according to a recent study published in JAMA Internal Medicine.
 02.06.2026
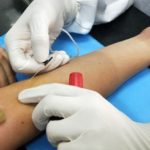
02.06.2026Screening all young people for a genetic form of dangerously high cholesterol could prevent heart attacks and strokes later in life, but would not be cost-effective under the current healthcare system, according to a new modelling study published in JAMA.
 01.13.2026
01.13.2026Lurie Cancer Center is pleased to announce a new group of leadership appointments supported by the NCI Cancer Center Support Grant, following the center’s recent NCI renewal and Exceptional rating—the highest distinction awarded by the National Cancer Institute.
“These appointments reflect the depth of talent and leadership across our cancer center,” said Leonidas Platanias, MD, PhD, director of the Lurie Cancer Center. “The remarkable strengths and expertise of each individual will enhance our efforts in research, education, and clinical care, and I look forward to working with them in these important roles.”
 12.09.2025We are delighted to announce the finalists for the William T. Grant Scholars Program class of 2031. Eleven early-career researchers were selected from a pool of 153 applicants after a rigorous review by our staff and Selection Committee.
12.09.2025We are delighted to announce the finalists for the William T. Grant Scholars Program class of 2031. Eleven early-career researchers were selected from a pool of 153 applicants after a rigorous review by our staff and Selection Committee. 11.21.2025Designing a large-scale research study often requires creativity and a collaborative mindset. Fortunately, the all2GETHER team had both.
11.21.2025Designing a large-scale research study often requires creativity and a collaborative mindset. Fortunately, the all2GETHER team had both. 09.23.2025
09.23.2025A novel approach to detect RNA modification patterns in patient blood samples may be a promising tool for the early detection of colon cancer, as detailed in a recent study published in Nature Biotechnology.
 09.11.2025
09.11.2025A cardiovascular disease risk prediction tool developed by Northwestern Medicine scientists may also be effective for identifying which patients most benefit from statin therapy, according to a recent study published in JAMA Cardiology.
 09.10.2025
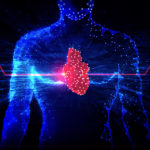
09.10.2025Scientists have discovered more than 100 new epigenetic biomarkers that may help predict cardiovascular disease risk and inform preventive care measures to improve long-term outcomes, according to a recent study published in Circulation.
 09.04.2025
09.04.2025An international multi-center study revealed how diet plays a greater role in the prevalence of obesity globally than was previously understood, according to findings published in the Proceedings of the National Academy of Sciences.
 07.16.2025
07.16.2025A new risk prediction tool developed by the American Heart Association (AHA) estimated cardiovascular disease (CVD) risk in a diverse patient cohort more accurately than current models, according to a recent study published in Nature Medicine.
 07.03.2025
07.03.2025Poor prepregnancy cardiovascular health is associated with a higher risk of developing gestational diabetes and coronary artery calcium in midlife, according to a recent Northwestern Medicine study.
 07.03.2025Kennedy said his vision is for every American to have a wearable within 4 years. Nabil Alshurafa, PhD shares his insights on the benefits and risks of the emerging technology.
07.03.2025Kennedy said his vision is for every American to have a wearable within 4 years. Nabil Alshurafa, PhD shares his insights on the benefits and risks of the emerging technology. 07.03.2025A new algorithm developed by the HABits Lab enabled smartwatch fitness trackers to more accurately estimate energy expenditure by individuals with obesity.
07.03.2025A new algorithm developed by the HABits Lab enabled smartwatch fitness trackers to more accurately estimate energy expenditure by individuals with obesity. 06.24.2025Nabil I Alshurafa, PhD and his lab, the HABits Lab, recently developed a new algorithm that enables smart watches to more accurately monitor the calories burned by people with obesity during various physical activities. Read their Nature Scientific Report or watch their video to learn more.
06.24.2025Nabil I Alshurafa, PhD and his lab, the HABits Lab, recently developed a new algorithm that enables smart watches to more accurately monitor the calories burned by people with obesity during various physical activities. Read their Nature Scientific Report or watch their video to learn more. 04.29.2025
04.29.2025Norrina Bai Allen, PhD, vice chair for Research of the Department of Preventive Medicine and Quentin D. Young Professor of Health Policy, has been named the Director of the Center for Health Services and Outcomes Research (CHSOR).
 03.30.2025
03.30.2025Spearheading the team from the Center for Global Oncology are Lifang Hou, MD, PhD, center director, and Mamoudou Maiga, MD, PhD, center associate director.
 02.28.2025
02.28.2025Mercedes Carnethon, PhD, takes the baton as the new chair of Preventive Medicine.